Syphilis and HIV have a well-documented connection, with each infection increasing the risk and severity of the other. Syphilis, caused by the bacterium Treponema pallidum, has been on the rise globally, with health experts warning of its impact on HIV transmission.
Medical research confirms that syphilis makes it easier to acquire and transmit HIV, while HIV alters the course of syphilis, sometimes making it more aggressive.
Dr. Gail Bolan, a public health expert, states, “Genital sores caused by syphilis make it easier to transmit and acquire HIV. There is an estimated 2- to 5-fold increased risk of acquiring HIV if exposed while syphilis is present.”
Understanding this link is crucial for public health efforts aimed at reducing both infections. Below, we explore how syphilis increases the risk of HIV, how HIV affects syphilis progression, and what can be done to prevent and manage co-infections.
Key Takeaways
- Syphilis makes it easier to acquire and transmit HIV.
- HIV worsens syphilis progression and may cause treatment challenges.
- Routine testing and early treatment are crucial to breaking the cycle of co-infection.
- Condoms, PrEP, and safer sex practices reduce both syphilis and HIV risk.
How Syphilis Increases HIV Risk
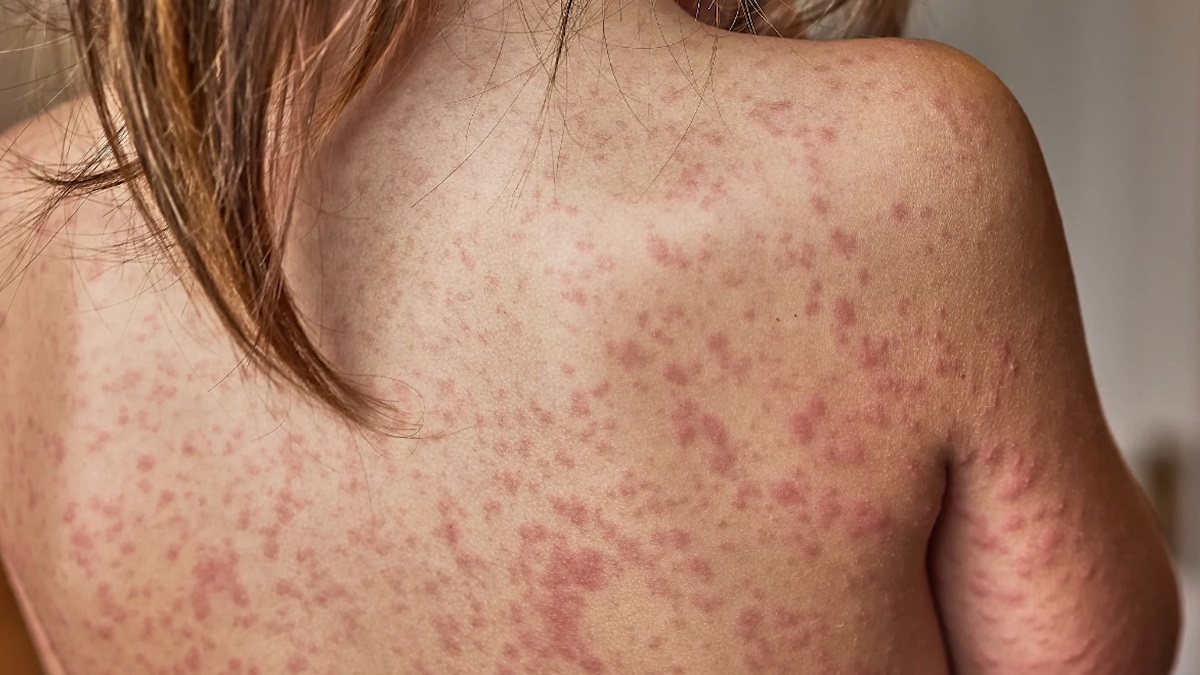
Syphilis significantly raises the likelihood of acquiring HIV. The presence of syphilitic sores or ulcers creates open entry points for HIV, allowing the virus to enter the body more easily. The immune response to syphilis also increases the number of CD4+ T cells in affected areas—the very cells HIV targets.
According to a study published in The Lancet, individuals with syphilis are nearly three times more likely to contract HIV compared to those without syphilis.
A CDC report states, “Having a sore or break in the skin from an STI such as syphilis may allow HIV to more easily enter your body.”
Syphilis also increases the risk of transmitting HIV. If an HIV-positive person has syphilis, their viral load can spike, making them more infectious. Medical studies confirm that HIV-positive individuals with syphilis experience a temporary increase in HIV viral load and a decline in immune function, further amplifying the risk of transmission.
How HIV Affects Syphilis Progression
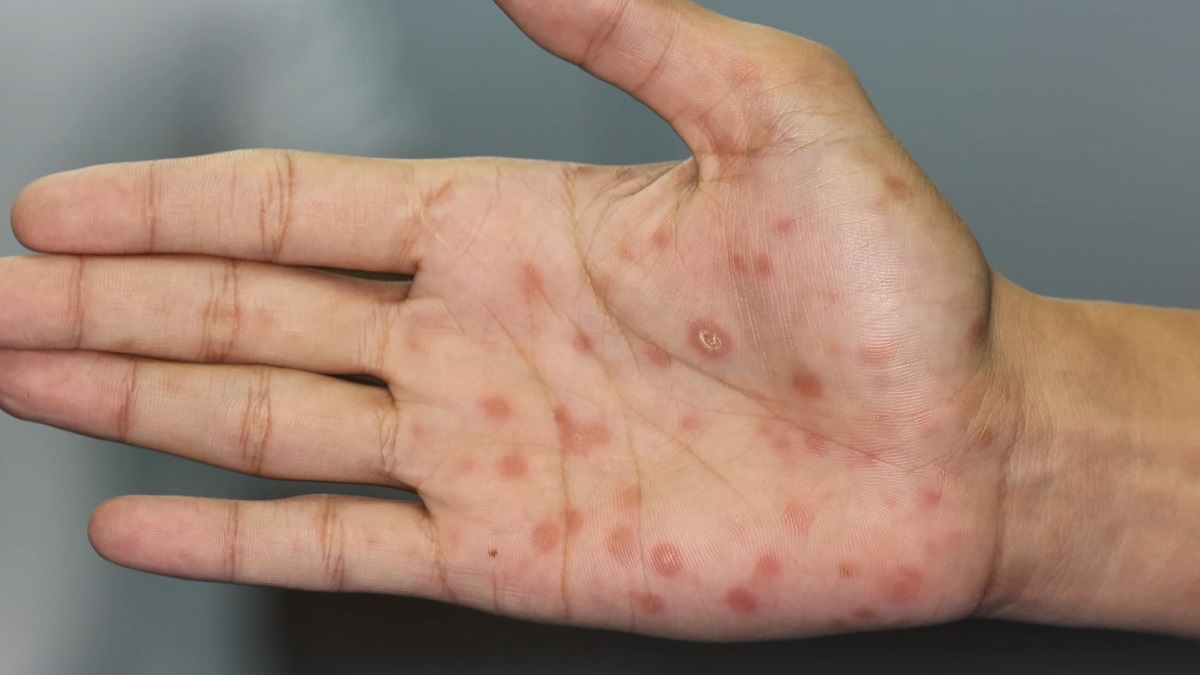
HIV infection can alter the way syphilis progresses, often making it more aggressive or harder to treat. Research shows that HIV-positive individuals are more likely to develop neurosyphilis, a serious condition where syphilis affects the nervous system. Persons with HIV infection who have early syphilis might be at increased risk for neurologic complications.
HIV can also cause atypical syphilis symptoms, making it harder to diagnose. Instead of the usual progression of syphilis through stages, co-infected individuals may experience overlapping symptoms, making clinical evaluation challenging. Some may even show false-negative syphilis test results due to immune system changes caused by HIV.
Furthermore, treatment response differs in HIV-positive patients. While penicillin remains the standard treatment for syphilis, research suggests that co-infected individuals are at a higher risk of treatment failure, requiring more intensive follow-up testing.
Medical Insights Into Syphilis-HIV Co-Infection
Several biological mechanisms explain why they reinforce each other:
- Mucosal Disruption: Syphilis ulcers allow HIV to enter the body more easily.
- Increased Inflammation: Syphilis-related inflammation attracts HIV target cells, making infection more likely.
- Viral Load Surge: Syphilis co-infection can cause temporary HIV viral load increases, making HIV-positive individuals more infectious.
- Weakened Immune Response: HIV weakens the immune system, allowing syphilis to spread more aggressively.
Experts describe this as a syndemic, meaning the two infections amplify each other’s effects, worsening public health outcomes.
Prevention Strategies
Given the strong link between syphilis and HIV, prevention efforts must target both infections simultaneously. Effective strategies include:
1. Routine Testing and Early Diagnosis

Regular screening helps detect infections early, allowing for timely treatment. The CDC recommends that anyone diagnosed with syphilis should be tested for HIV, and vice versa.
2. Prompt Treatment and Partner Notification
Syphilis is curable with antibiotics, but delayed treatment increases the risk of HIV transmission. Public health programs focus on partner notification, ensuring that sexual partners of infected individuals get tested and treated to prevent further spread.
3. Condom Use and Safe Sex Practices
Condoms reduce the transmission of both syphilis and HIV. While syphilis sores may sometimes occur outside condom-covered areas, consistent condom use lowers infection risk significantly.
4. HIV Pre-Exposure Prophylaxis (PrEP) and Preventive Therapies
PrEP is a daily pill that reduces HIV risk by up to 99%. The CDC states that individuals diagnosed with syphilis should be offered PrEP to prevent subsequent HIV infection.
Emerging research also suggests that doxycycline post-exposure prophylaxis (doxy-PEP) can reduce syphilis transmission when taken after high-risk sexual encounters.
5. Education and Community Outreach
Public awareness is essential. Community health programs provide free STI testing, safer sex education, and PrEP access to high-risk populations.
Public Health Implications
The rise of syphilis poses a direct threat to HIV control efforts. Health officials stress that syphilis prevention is also HIV prevention. Addressing the intersection of these infections requires:
- Integrated Sexual Health Services: Clinics should offer dual syphilis/HIV testing and immediate linkage to treatment.
- Reducing Stigma: Stigma prevents people from seeking care. Public health campaigns must normalize routine STI testing.
- Targeted Interventions: Surveillance programs track high-risk populations and deploy rapid response teams to contain outbreaks.
WHO Director-General Dr. Tedros Adhanom Ghebreyesus warned, “The rising incidence of syphilis raises major concerns.” Global health efforts must scale up prevention and treatment services to curb both syphilis and HIV.
Conclusion
Both diseases fuel each other’s spread, making co-infection a critical public health challenge. Syphilis increases HIV risk through open sores and inflammation, while HIV alters syphilis progression and complicates treatment. Early detection, timely treatment, and preventive measures are essential to breaking the cycle of transmission.
Experts emphasize that every syphilis infection prevented is a potential HIV case avoided. Strengthening STI and HIV prevention efforts will not only reduce cases of both infections but also improve overall public health outcomes.
Addressing this dual epidemic requires integrated healthcare strategies, ongoing community education, and expanding access to testing, treatment, and prevention tools.
References
- National Institutes of Health – Effect of syphilis infection on HIV acquisition: a systematic review and meta-analysis
- hiv.org – Syphilis and HIV: A Dangerous Duo Affecting Gay and Bisexual Men
- The Lancet – Syphilis and HIV: a dangerous combination
- Research Online – Neurosyphilis in HIV
- National Library of Medicine – Secondary Syphilis in the Spotlight: Atypical Cutaneous Manifestation Overshadowing Kaposi Sarcoma in a Newly Diagnosed HIV Patient
- National Library of Medicine – Treatment of Syphilis A Systematic Review
- National Library of Medicine – Mechanisms of sexually transmitted infection‐induced inflammation in women: implications for HIV risk
- National Library of Medicine – The immunological response to syphilis differs by HIV status; a prospective observational cohort study